We’ve all heard the term inflammation, especially when dealing with an injury. But what exactly is it, and why does it happen? Inflammation is the body’s natural response to damage, causing pain, swelling, heat, and redness in the affected area. It might seem like an inconvenience, but inflammation plays a crucial role in healing.
When we experience pain due to inflammation, the first instinct is often to get rid of it as quickly as possible. A couple of anti-inflammatories like ibuprofen, and problem solved, right?
Wrong.
While reducing pain may seem like the best solution, inflammation isn’t just an unfortunate side effect of injury—it’s a necessary process. The pain tells us something is wrong, preventing us from worsening the injury. The swelling and increased blood flow deliver white blood cells to the damaged tissue, aiding in repair and clearing out cellular debris. When we interfere with this process by taking anti-inflammatories too soon, we may actually be slowing down healing rather than helping it.
Of course, anti-inflammatories can be useful in certain situations, but relying on them too soon can cause more harm than good. Pain exists for a reason—it stops us from pushing an injured area too hard, too soon. If we mask the pain before the tissue has had a chance to recover properly, we increase the risk of re-injury, which can lead to a longer and more complicated recovery. Beyond that, disrupting the body’s natural inflammatory response can sometimes lead to an exaggerated inflammatory state, meaning instead of resolving inflammation, we may actually prolong it. This can result in chronic pain, tissue damage, and long-term dysfunction.
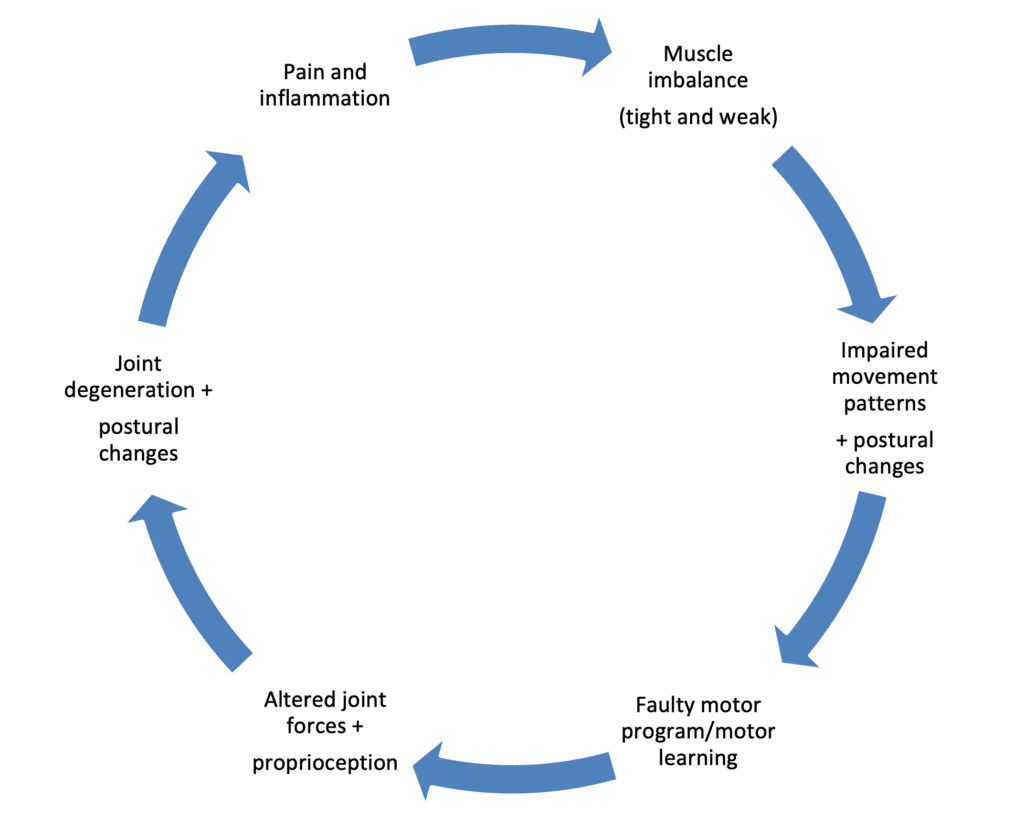
But if we shouldn’t suppress inflammation entirely, how do we manage it in a way that allows healing to continue? Instead of shutting down the inflammatory process completely, we can use strategies that help regulate it while still allowing the body to do what it needs to do. A good example of this is the R.I.C.E. protocol—rest, ice, compression, and elevation.
These methods help to manage pain and swelling without completely halting the body’s healing mechanisms. Resting prevents further damage, ice reduces excessive swelling, compression supports the injured area, and elevation minimises fluid build-up.
There are also alternative therapies that can help modulate inflammation and support the body’s healing process. Manual thera
pies such as physiotherapy, osteopathy, and massage can improve circulation and support tissue repair. Acupuncture has been shown to help regulate the body’s inflammatory response, and topical anti-inflammatory creams can provide localised relief without the systemic effects of oral medications. These approaches help to manage inflammation in a way that doesn’t interfere with the body’s natural repair process.
So if inflammation is such an important part of healing, how does it become chronic? And what can we do to prevent the body from getting stuck in a prolonged inflammatory state?
We’ll explore that in the next blog… Stay tuned.
Disclaimer: This post is for general information only and is not a substitute for personalised medical advice. If you’re experiencing recurring or concerning symptoms, especially neurological ones and or severe uncharacteristic headaches, please speak to your GP or seek urgent medical care. Social media isn’t a diagnosis tool, even when it’s run by a qualified health professional.